Cardioversion
Cardioversion refers to the process of restoring the normal heart rhythm from an abnormal rhythm. Most elective cardioversions are performed to treat atrial fibrillation or atrial flutter – heart rhythm disturbances that originate in the upper chambers (atria) of the heart.
Why do I need a cardioversion?
Normally, each heartbeat starts in the upper right chamber (right atrium) of the heart in a region containing specialised “pacemaker” cells. Each time these cells fire (usually 1 to 2 times per second) this electrical impulse is transmitted in an organised fashion throughout the heart resulting in a coordinated rhythmic heartbeat. In patients with atrial fibrillation, instead of the normal organised electrical activity, the atria fibrillate (or quiver) because of chaotic electrical activity that circulate throughout both atria. This can result in less efficient blood pumping and an irregular or fast heartbeat.
WHAT ARE THE DIFFERENT TYPES OF CARDIOVERSION?
Cardioversion can be chemical or electrical. Chemical cardioversion refers to taking anti-arrhythmia medication to restore the heart’s rhythm to normal. Such medications work by altering the heart’s electrical properties to suppress the abnormal heart rhythms and restore a normal rhythm. These medications are usually given as an outpatient but sometimes you may be admitted to hospital for this therapy. Electrical cardioversion (also known as direct-current or DC cardioversion) is a procedure whereby an electrical current (shock) is delivered through the chest wall to the heart under anaesthesia. The shock is delivered through special electrodes or paddles on the chest and sometimes the back. The purpose of the cardioversion is to interrupt the abnormal electrical circuit(s) in the heart and to restore a normal heartbeat. The delivered shock causes all the heart cells to contract simultaneously, thereby interrupting and terminating the abnormal electrical rhythm (typically fibrillation of the atria) without damaging the heart. The heart’s electrical system then restores a normal heartbeat.
THE CARDIOVERSION PROCEDURE
The electrical cardioversion is performed in the angiography suite, coronary care unit or recovery room. It is necessary for you to fast for at least 6 hours prior to the cardioversion. You can take your usual medications on the morning of the procedure with a small amount of water. In many cases you will have been on warfarin prior to the cardioversion. It is important that the level of the blood thinning (the INR) is checked prior to the cardioversion, usually the day prior or the morning of the procedure. Your cardioversion will only be performed if you have had a minimum of 3 weeks whereby your INR has been between 2 and 4. If this has not been the case it is vital that you notify the staff undertaking the cardioversion. Occasionally, a trans-esophageal echocardiogram (TOE) will be performed prior to cardioversion. This is usually done when there is a high index of suspicion of clots inside the heart or your warfarin level has been fluctuating.
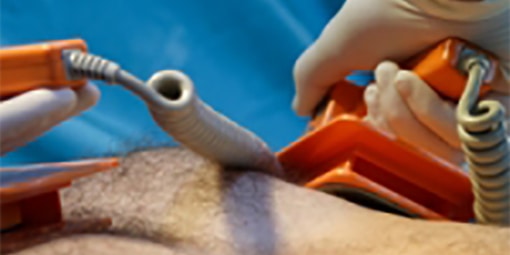
For the cardioversion, special pads are used to minimise any skin burning or irritation from the electrical shock. You will be connected to an external defibrillator to allow monitoring of your heart rhythm and to allow the application of the necessary energy to restore your heart’s rhythm back to normal. As the shock may be uncomfortable, some form of sedation or anesthesia is administered intravenously. Once you are sedated, the shock is delivered. Additional shocks at higher energy levels can be delivered if the first shock does not restore the rhythm back to normal. The success rate depends upon a number of factors but there is an approximately 90% chance that the normal rhythm (sinus rhythm) will be restored. In a proportion of patients, the arrhythmia subsequently recurs and repeated cardioversion may be required. Patients generally wake quickly and without any recollection of the shocks because of the effects of the sedatives. It is crucial that warfarin is continued (maintaining the INR between 2 and 4) for at least a month after the procedure. You will not be able to drive yourself home from the procedure and will need a responsible adult to stay with you overnight after the procedure. You should not drive or make any important decisions for 24 hours after the procedure.
CARDIOVERSION RISKS
Cardioversion is a very safe and effective treatment for atrial fibrillation and atrial flutter. However, there are some potential complications. Stroke (or embolism) is perhaps the most dreaded complication. This is where a blood clot is dislodged from the heart into the blood stream. If the clot travels to a major organ it can cause problems such as a stroke or heart attack. For this reason if the atrial fibrillation has been present for more than 48 hours, or its duration is unknown, either the blood must be thinned using warfarin for at least 3 weeks or you must undergo TOE examination prior to the cardioversion. If adequate blood thinning is undertaken the risk of an embolus is less than 1:1000. Depending on how long you have been in atrial fibrillation or flutter, your normal pacemaker may not function immediately on terminating the abnormal rhythm. Usually this recovers promptly but in rare cases temporary and sometimes permanent pacemakers may need to be inserted. Finally, there is a very small risk associated with the administration of the sedation required for the cardioversion, but the likelihood of a significant anaesthetic complication is also less than 1:1000.
